Osteoarthritis of Knee
Anatomy of the Knee Joint
 The knee joint is commonly referred to as a "hinge" joint because it allows the knee to flex and extend. The knee joint includes the end of the thigh bone (the femur), the top of the leg bone (the tibia) and the knee cap (the patella). A smooth cushion of articular cartilage covers the end surfaces of both of these bones so that they slide against one another smoothly. The patella, or kneecap, is the moveable bone on the front of the knee.
The knee joint is commonly referred to as a "hinge" joint because it allows the knee to flex and extend. The knee joint includes the end of the thigh bone (the femur), the top of the leg bone (the tibia) and the knee cap (the patella). A smooth cushion of articular cartilage covers the end surfaces of both of these bones so that they slide against one another smoothly. The patella, or kneecap, is the moveable bone on the front of the knee. What happens in Arthritis?
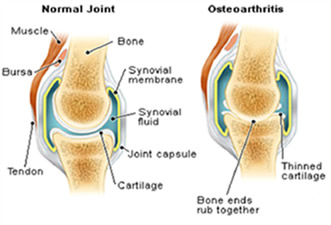 In this condition, the articular cartilage, which is the smooth gliding surface of the joint, wears away and the bones grind against each other, creating popping sounds, pain and loss of normal movement. This condition occurs primarily in people over 50 and is the most common form of arthritis.
In this condition, the articular cartilage, which is the smooth gliding surface of the joint, wears away and the bones grind against each other, creating popping sounds, pain and loss of normal movement. This condition occurs primarily in people over 50 and is the most common form of arthritis. - Another common type of arthritis that can affect the knees is Rheumatoid Arthritis. It is caused by dysfunction of the immune system and the patients can have morning stiffness and affection of multiple joints in the body like knees, hips, wrists, hands, spine etc.
- Trauma-related arthritis results when a joint is injured, either by fracture, dislocation or damage to the ligaments surrounding the joint causing Instability or damage to the joint surface.
What are the signs and symptoms of Osteoarthritis?
- Severe knee pain that limits everyday activities, including walking, going up and down stairs, and standing up from a chair. The patient may find it hard to walk longer distances without significant pain and may need to use a stick or walker.
- Moderate or severe knee pain while resting, day or night.
- Chronic knee inflammation and swelling that doesn't improve with rest or medications.
- Knee deformity a bowing in or out of the knee.
- Knee stiffness- inability to bend and straighten the knee.
How is knee Arthritis diagnosed?
Osteoarthritis is diagnosed by taking detailed history of the patient and examination to assess knee motion, stability and strength and overall leg alignment. X-rays are taken to determine the extent of damage and deformity in the arthritic knee. Occasionally blood tests, an MRI (magnetic resonance imaging) etc. may be needed to determine the condition of the bone and soft tissues of the knee. Front x-ray views of a normal and arthritic knee are shown in Figures 1A and 1B respectively. The thigh bone (femur) is on the top and the leg bone (tibia) is on the bottom. The apparent space between the bones is actually occupied by articular cartilage which is not dense enough to be seen on x-ray and is called the joint space. In advanced arthritis, the articular cartilage has been completely worn away and the bone of the femur and tibia, and the femur and patella, come into direct contact. Wear of articular cartilage can be seen on x-rays as a decrease in the space between the bones.
Front x-ray views of a normal and arthritic knee are shown in Figures 1A and 1B respectively. The thigh bone (femur) is on the top and the leg bone (tibia) is on the bottom. The apparent space between the bones is actually occupied by articular cartilage which is not dense enough to be seen on x-ray and is called the joint space. In advanced arthritis, the articular cartilage has been completely worn away and the bone of the femur and tibia, and the femur and patella, come into direct contact. Wear of articular cartilage can be seen on x-rays as a decrease in the space between the bones.What are the different treatment options for Osteoarthritis?
Osteoarthritis in majority of the patients is a degenerative condition due to aging process and as the age advances, it progresses leading to increase in pain and stiffness of the joint.Non-Surgical Treatment
- This treatment is given in very early cases of osteoarthritis or if the patient does not want to undergo surgery.
- Strenuous and painful activities should be avoided. Gentle exercise such as walking or swimming can be adopted.
- The patient may benefit from some moist heat, massage or other forms of physical therapy.
- Weight loss can be very helpful in reducing pain from arthritic knees by reducing the stress.
- Pain killers or anti-inflammatory medication do not alter the arthritis in the knee but help to reduce the pain and inflammation. However, the patient should be careful to take Non steroidal anti-inflammatory agents like Ibuprofen, Diclofenac etc. as they have harmful effect on the kidney function. The patients suffering from Diabetes or Hypertension should be even more cautious.
- Certain medicines like Glucosamine Sulphate, Chondroitin Sulphate, Diacerin etc. are also used in early osteoarthritis to retard cartilage degeneration and treat arthritis. Though their use as a therapy for osteoarthritis appears safe, there is conflicting evidence as to their effectiveness.
- A cane or a crutch may be required in order to walk.
- There are also medicines that can be injected directly into the knee, such as cortisone and newer products such as Inj. Hyalgan or Synvisc that improve lubrication of the joint and may provide some pain relief. Unfortunately, the arthritis is progressive in most cases.
- Specialized Braces or Belts
- There are specialized braces that can be helpful in some cases of knee arthritis. These braces are designed to create a force which transfers load from an area of the knee where the cartilage is more worn, to an area of the knee where the cartilage is less worn.
- They are often tried in very young arthritic patients, those who have early arthritis or those patients who opt for non-surgical option before undergoing surgery.
- Though these braces are helpful in some cases, some patients find them very cumbersome to use. They are less likely to help in cases of advanced arthritis of knee joint.
Surgical Treatment
If the pain is not adequately controlled by the above measures, the surgeon considers following treatment options before advocating total knee replacement to the patient.
a) Arthroscopy
- Arthroscopy requires only small incisions around the knee which allow the insertion of small instruments, which are about the size of a pen or pencil.
- With arthroscopy, degenerated and worn cartilage can be trimmed and smoothed, which reduces the source of inflammation. Additionally, the lining of the knee (the synovium), can be trimmed, and this also decreases inflammation.
- Patients who have knee arthroscopy require staying in hospital just for a day. Recovery from surgery occurs over a couple of weeks.
- Unfortunately, the benefit of arthroscopy decreases as the degree of arthritis increases.
- In advanced arthritis, arthroscopy is of little value.
b) Osteotomy
- In some cases of knee joint arthritis, where the leg is imperfectly aligned, they can be treated by an osteotomy.
- An osteotomy is an operation that cuts the bone usually below the knee, and re-aligns the knee to a better position. This is a bigger operation than an arthroscopy and patients usually stay for 2-3 days in the hospital.
- It takes 6 to 8 weeks for the bone to heal. Physical therapy is usually required to restore knee motion and strength. Complete recovery takes a number of months.
- An osteotomy is a good operation, especially for younger patients, and those where the leg is clearly not straight and the cartilage wear is confined to one portion of the knee.
- Unfortunately, the success of an osteotomy decreases as the degree of arthritis increases.
c) Uni-Compartmental Arthroplasty
- In a few cases, only a portion of the knee joint surfaces have worn out and need to the replaced. When only a portion of the knee is replaced, this is called a uni-compartmental arthroplasty.
- Patients usually stay 3 or 4 days in the hospital and it takes a couple of months for the knee to recover. Physical therapy is usually required to restore knee motion and strength.
- Unfortunately, in most cases of arthritis, the joint surfaces are diffusely worn. Uni-compartmental arthroplasty is, therefore, less commonly performed than total knee replacement.